- 翰林提供学术活动、国际课程、科研项目一站式留学背景提升服务!
- 400 888 0080
AQA A Level Biology复习笔记8.2.11 Tumour Development
Tumour Development
- Cancers demonstrate how important it is that cell division is precisely controlled, as cancers arise due to uncontrolled mitosis
- Cancerous cells divide repeatedly and uncontrollably, forming a tumour (an irregular mass of cells)
- Cancers start when the expression of genes that control cell division changes. If the mutated gene is one that causes cancer it is referred to as an oncogene
- Mutations are common events and don’t lead to cancer most of the time
- Most mutations either result in early cell death or result in the cell being destroyed by the body’s immune system
- As most cells can be easily replaced, these events usually have no harmful effect on the body
- The mutations that result in the generation of cancerous cells do not result in early cell death or in the cell being destroyed by the body’s immune system
- This means that the harmful mutation occurring in the original cell can be passed on to all that cell’s descendants
- A typical tumour contains around a thousand million cancerous cells by the time it is detected
- Carcinogens are any agents that may cause cancer (eg. UV light, tar in tobacco smoke and X-rays). If the agent causes cancer it is described as carcinogenic
Tumour suppressor genes
- Tumour suppressor genes are normal genes that code for proteins that regulate the cell cycle
- The proteins encoded for by tumour suppressor genes carry out the following functions:
- DNA repair
- Slowing the cell cycle by ensuring checks are made
- Signalling apoptosis (cell death) when the cell is faulty
- These proteins ensure that cells do not replicate if they contain mutated DNA or are faulty as these characteristics can lead to tumour formation
- Tumours develop if tumour suppressor genes are mutated or silenced
- A mutation can be any of the mutations learnt in topic 8.1 that results in a non-functional protein
- Silencing can occur through epigenetic changes and RNAi
- Hypermethylation of DNA (over-addition of methyl groups to cytosine nucleotides) causes transcription-inhibiting proteins to bind the DNA, if this occurs around tumour suppressor genes this could result in tumour development as the necessary regulatory proteins coded for by tumour suppressor genes will not be produced
- RNA interference by siRNAs targeting tumour suppressor genes for breakdown can also lead to tumour development for the same reason
- BRCA-1 is an example of a human tumour suppressor gene expressed mainly in breast tissue
- The role of the BRCA-1 protein is to repair broken or mutated DNA
- If the BRCA-1 protein cannot repair the DNA it signals for apoptosis to begin
- In breast cancers, inhibition of BRCA-1 expression leads to a lack of DNA repair and apoptosis, leading to the formation of cancerous tumours
Oncogenes
- Proto-oncogene are normal genes that code for proteins that regulate cell growth (growth factors) and cell differentiation
- Proto-oncogenes can mutate to become oncogenes
- Mutation occurs because of carcinogens such as exposure to UV, X-rays and smoking to name a few examples
- Oncogenes are mutated genes that have the ability to cause cancer through the deregulation of cell growth
- Mutations that produce oncogenes usually causes the proteins that stimulate cell growth and division to be constantly activated
- When these proteins are activated, the cell cycle is sped up
- If the proteins involved in apoptosis are also mutated, this can lead to tumour formation
- Mutations of proto-oncogenes to produce oncogenes can occur through inversion or translocation mutations where an activating segment of a gene is attached to a proto-oncogene leading to either:
- Gene expression being upregulated
- The protein produced being constantly activated (unable to be switched off)
- Within cells there are common ways in which proteins are activated/deactivated, these include:
- Phosphorylation - the addition of a phosphate group from ATP
- Complex formation - binding to another protein or coenzyme which changes the protein's conformation, potentially opening up another binding site or revealing an active site
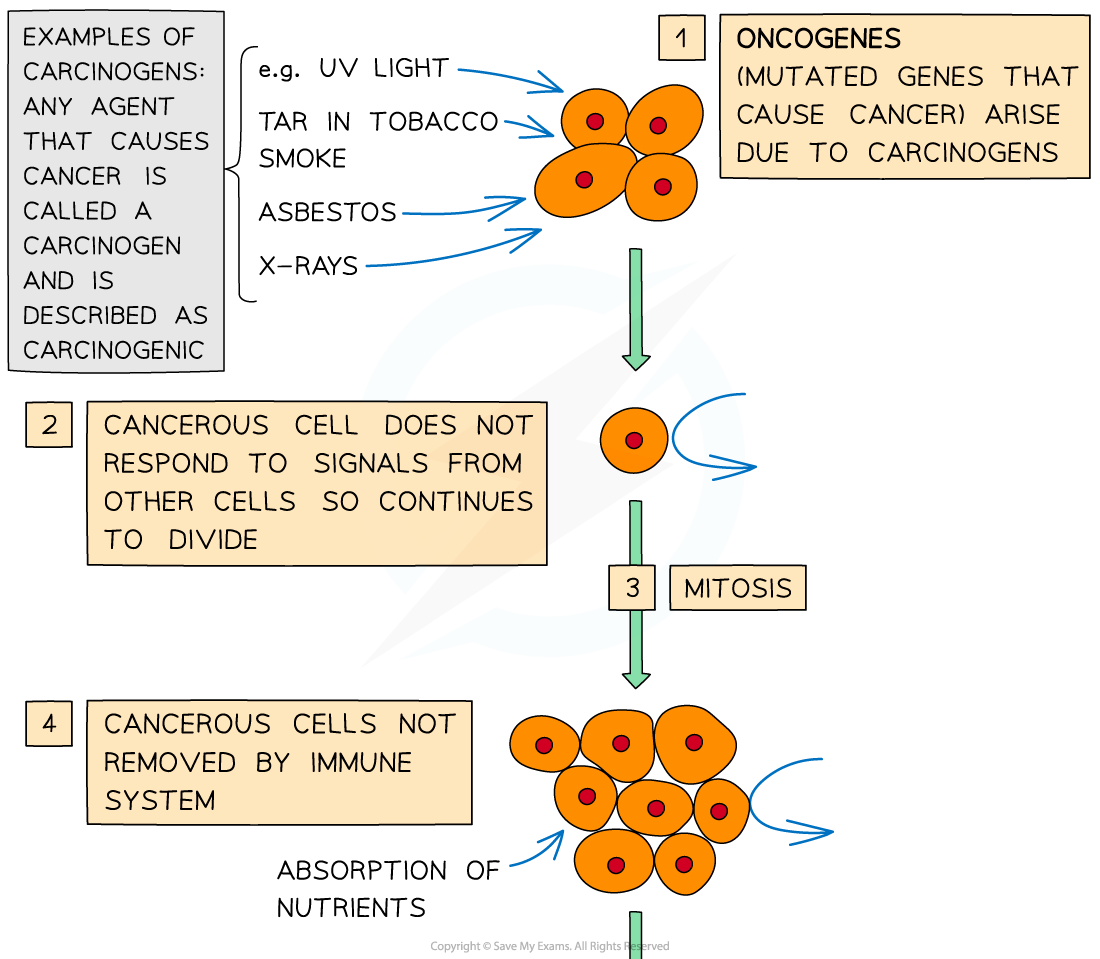
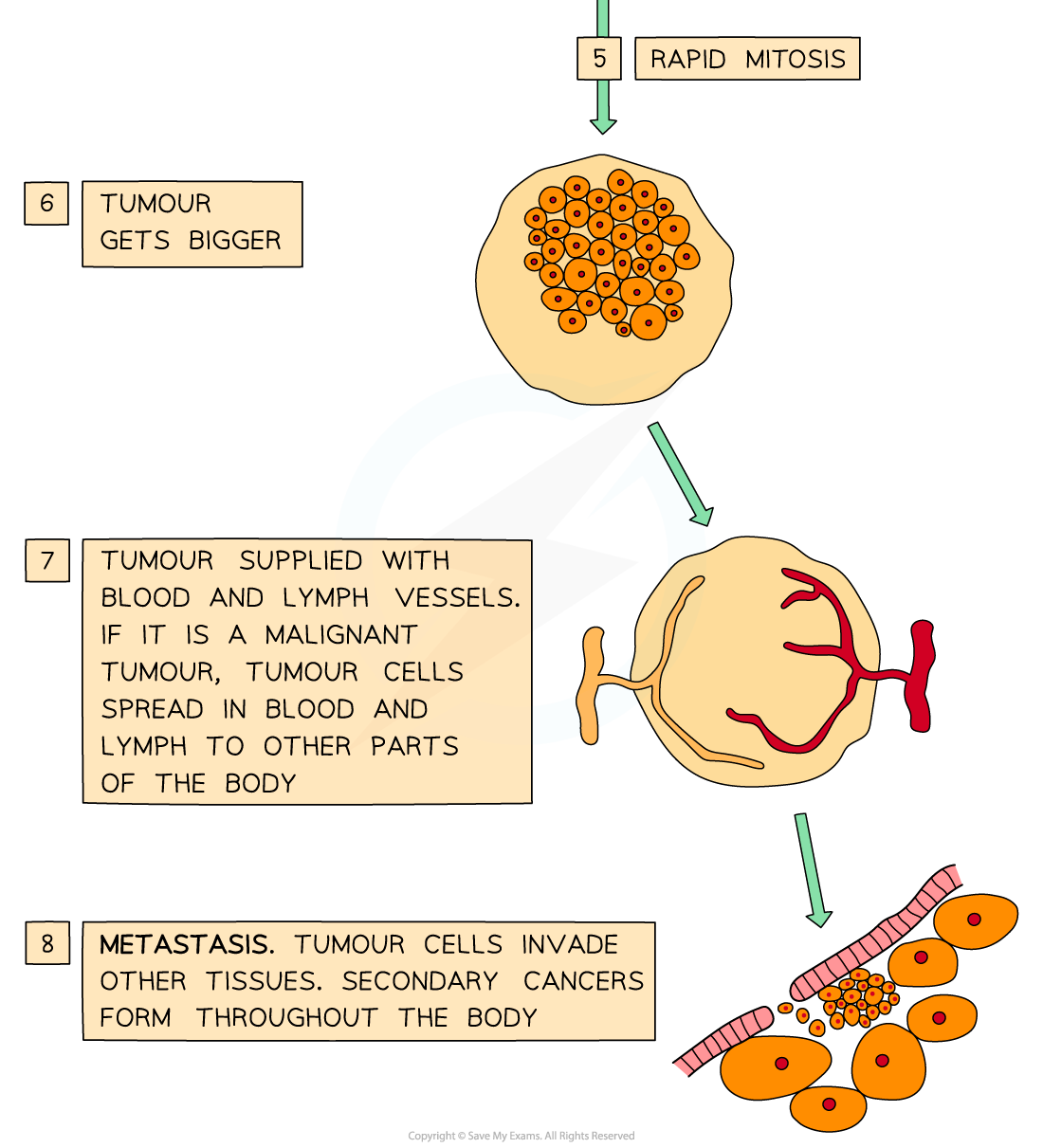
Several processes must occur in order for metastatic cancer to develop
Oestrogen-dependent breast tumours
- Oestrogen is a steroid hormone that upregulates transcription of certain genes through the stimulation of the ERα oestrogen receptor
- High concentrations of oestrogen can lead to the development of breast cancer
- High concentrations can be a result of over-expression of the oestrogen gene or from supplementary oestrogen taken in medication
- About 70% of breast tumours are categorised as oestrogen receptor-positive, these breast tumours are also called oestrogen-dependent breast tumours
- Oestrogen is needed by these tumours to stimulate the expression of cell cycle genes that lead to growth and replication
- The cancer cells within these tumours have oestrogen receptors that promote cell growth when stimulated by oestrogen
- The genes are switched on through the oestrogen dependent gene expression pathway in which oestrogen diffuses into the cell and through a nuclear pore until it reaches the oestrogen receptors
- The main treatment of this type of tumour is a drug called tamoxifen which has a similar chemical structure to oestrogen and therefore acts as a competitive inhibitor
- This means that tamoxifen permanently binds to oestrogen receptors, stopping oestrogen from binding and therefore inhibiting the receptor's action
- So the genes that are usually upregulated by oestrogen are not expressed as the oestrogen receptor cannot bind to the promoter
- Therefore, tumours cannot grow
Exam Tip
In the exam, you could be asked to evaluate evidence showing correlations between genetic and environmental factors and various forms of cancer. Questions like these often look at the use of control groups and how a certain risk factor can be linked to genetic mutation which then leads to faulty or upregulated proteins which cause cancer. You may also be asked to use your knowledge of oncogenes and tumour suppressor genes, as well as the epigenetic and post-transcription mechanisms within cells, to infer how they could be used in the prevention, treatment and cure of cancer.
转载自savemyexams
站内搜索
竞赛真题免费下载(点击下载)
在线登记
最新发布
© 2024. All Rights Reserved. 沪ICP备2023009024号-1





